World Journal of Emergency Medicine ›› 2022, Vol. 13 ›› Issue (3): 208-214.doi: 10.5847/wjem.j.1920-8642.2022.052
• Original Articles • Previous Articles Next Articles
Hong-li Xiao1, Lian-xing Zhao2, Jun Yang3, Nan Tong3, Le An3, Guo-xing Wang1, Miao-rong Xie1( ), Chun-sheng Li1(
), Chun-sheng Li1( )
)
Received:2021-10-10
Accepted:2022-02-20
Online:2022-05-13
Published:2022-05-01
Contact:
Miao-rong Xie,Chun-sheng Li
E-mail:lcscyyy@163.com;yyyyxmr@ccmu.edu.cn
Hong-li Xiao, Lian-xing Zhao, Jun Yang, Nan Tong, Le An, Guo-xing Wang, Miao-rong Xie, Chun-sheng Li. Increasing angiotensin-converting enzyme (ACE) 2/ACE axes ratio alleviates early pulmonary vascular remodeling in a porcine model of acute pulmonary embolism with cardiac arrest[J]. World Journal of Emergency Medicine, 2022, 13(3): 208-214.
Add to citation manager EndNote|Ris|BibTeX
URL: http://wjem.com.cn/EN/10.5847/wjem.j.1920-8642.2022.052
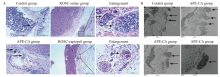
Figure 1.
Morphological and ultrastructure evaluation of pulmonary artery in APE. A: morphological evaluation of pulmonary artery in APE. Pulmonary arteries were occluded in the APE-CA and ROSC-saline groups (black arrow, ×100); fewer pulmonary arteries were occluded in the ROSC-captopril group (×100); plexiform lesions in the ROSC-saline group (enlargement, black arrows, ×400) and concentric lesions in ROSC-captopril group (enlargement, black arrows, ×400) were found. B: ultrastructure of endothelial cells in APE. Normal endothelial cell structure in the control group (black arrows, ×7,000), endothelial cell migration into vascular lumen in the APE-CA group (black arrows, ×10,000), and endothelial cell apoptosis in the APE-CA group (black arrows, ×10,000 and ×30,000). APE: acute pulmonary embolism; ROSC: return of spontaneous circulation; CA: cardiac arrest.
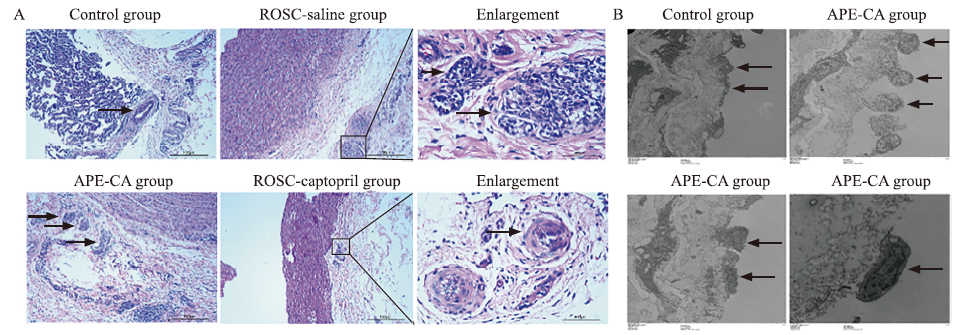
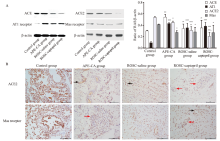
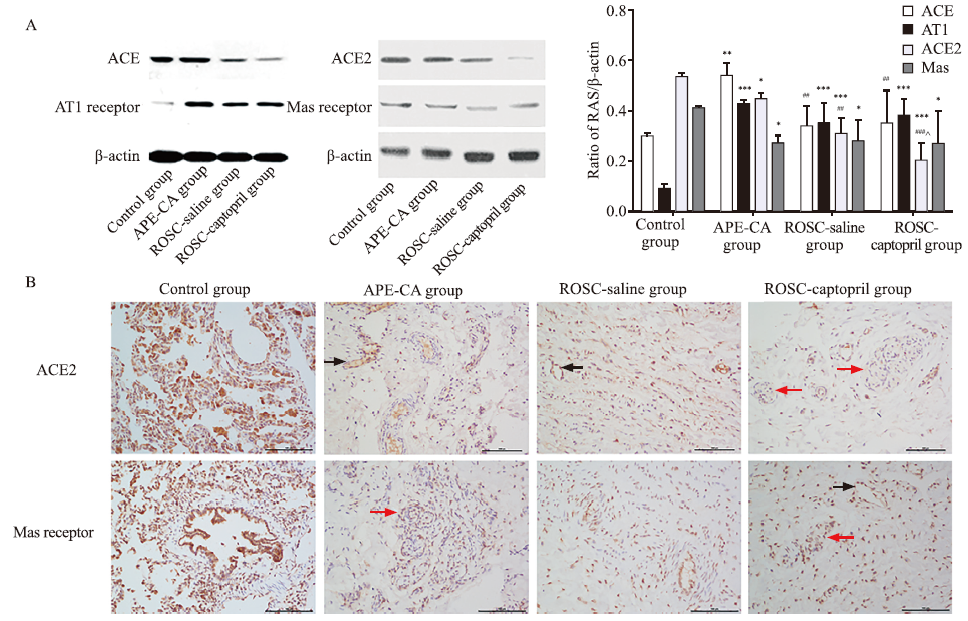
Figure 2.
Protein expression of RAS in the pulmonary artery and effects of captopril on APE. A: protein expression and quantitative analysis of RAS in the pulmonary artery and effects of captopril on APE, as revealed by Western blotting analysis; B: immunohistochemistry analysis of protein expression of ACE2 in the pulmonary artery in the control, APE-CA (black arrow pointing to expression of ACE2 in vascular endothelial cells), ROSC-saline (black arrow showing expression of ACE2 in vascular endothelial cells), and ROSC-captopril groups (red arrow showing expression of ACE2 in proliferative endotheliocytes); protein expression of Mas receptor in the pulmonary artery in the control, APE-CA (red arrow showing expression of Mas in proliferative endotheliocytes), ROSC-saline, and ROSC-captopril groups (black arrow showing expression of Mas receptor in vascular endothelial cells; red arrow showing expression of Mas receptor in proliferative endotheliocytes). Compared with the control group, *P<0.05, **P<0.01, ***P<0.001; compared with the APE-CA group, ##P<0.01, P<0.001; compared with the ROSC-saline group, ^P<0.05. Scale bar in B: 100 μm. RAS: renin angiotensin system; APE: acute pulmonary embolism; ACE2: angiotensin-converting enzyme 2; CA: cardiac arrest; ROSC: return of spontaneous circulation.
| 1 | Konstantinides SV, Meyer G, Becattini C, Bueno H, Geersing GJ, Harjola VP, et al. The Task Force for the diagnosis and management of acute pulmonary embolism of the European Society of Cardiology (ESC). 2019 ESC Guidelines for the diagnosis and management of acute pulmonary embolism developed in collaboration with the European Respiratory Society (ERS): the Task Force for the diagnosis and management of acute pulmonary embolism of the European Society of Cardiology (ESC). Eur Respir J. 2019; 54(3):1901647. |
| 2 |
Jia D, Ji C, Zhao M. Saddle pulmonary embolism is not a sign of high-risk deterioration in non-high-risk patients: a propensity score-matched study. World J Emerg Med. 2021; 12(4):261-7.
doi: 10.5847/wjem.j.1920-8642.2021.04.002 |
| 3 |
Dutta A, Tayal B, Kragholm KH, Masmoudi Y, Azizian J, McDonald L, et al. Characteristics and outcomes of cardiac arrest survivors with acute pulmonary embolism. Resuscitation. 2020; 155 6-12.
doi: 10.1016/j.resuscitation.2020.06.029 |
| 4 |
Smulders YM. Pathophysiology and treatment of haemodynamic instability in acute pulmonary embolism: the pivotal role of pulmonary vasoconstriction. Cardiovasc Res. 2000; 48(1):23-33.
pmid: 11033105 |
| 5 |
Bernard J, Yi ES. Pulmonary thromboendarterectomy: a clinicopathologic study of 200 consecutive pulmonary thromboendarterectomy cases in one institution. Hum Pathol. 2007; 38(6):871-7.
pmid: 17350667 |
| 6 |
Budhiraja R, Tuder RM, Hassoun PM. Endothelial dysfunction in pulmonary hypertension. Circulation. 2004; 109(2):159-65.
pmid: 14734504 |
| 7 | Morrell NW, Adnot S, Archer SL, Dupuis J, Lloyd Jones P, MacLean MR, et al. Cellular and molecular basis of pulmonary arterial hypertension. J Am Coll Cardiol. 2009; 54(1 Suppl):S20-S31. |
| 8 |
Orte C, Polak JM, Haworth SG, Yacoub MH, Morrell NW. Expression of pulmonary vascular angiotensin-converting enzyme in primary and secondary plexiform pulmonary hypertension. J Pathol. 2000; 192(3):379-84.
pmid: 11054722 |
| 9 |
Ji Y, Gao FY, Sun B, Hao J, Liu ZW. Angiotensin-converting enzyme Angiotensin-converting enzyme 2 inhibits apoptosis of pulmonary endothelial cells during acute lung injury through suppressing SMAD2 phosphorylation. Cell Physiol Biochem. 2015; 35(6):2203-12.
doi: 10.1159/000374025 |
| 10 |
Olkowicz M, Chlopicki S, Smolenski RT. Perspectives for angiotensin profiling with liquid chromatography/mass spectrometry to evaluate ACE/ACE2 balance in endothelial dysfunction and vascular pathologies. Pharmacol Rep. 2015; 67(4):778-85.
doi: 10.1016/j.pharep.2015.03.017 pmid: 26321281 |
| 11 |
Xiao HL, Li CS, Zhao LX, Yang J, Tong N, An L, et al. Captopril improves postresuscitation hemodynamics protective against pulmonary embolism by activating the ACE2/Ang-(1-7)/Mas axis. Naunyn Schmiedebergs Arch Pharmacol. 2016; 389(11):1159-69.
doi: 10.1007/s00210-016-1278-7 |
| 12 |
Pantazopoulos IN, Xanthos TT, Vlachos I, Troupis G, Kotsiomitis E, Johnson E, et al. Use of the impedance threshold device improves survival rate and neurological outcome in a swine model of asphyxial cardiac arrest. Crit Care Med. 2012; 40(3):861-8.
doi: 10.1097/CCM.0b013e318232d8de pmid: 21983368 |
| 13 |
Stadlbauer KH, Rheinberger K, Wenzel V, Raedler C, Krismer AC, Strohmenger HU, et al. The effects of nifedipine on ventricular fibrillation mean frequency in a porcine model of prolonged cardiopulmonary resuscitation. Anesth Analg. 2003; 97(1):226-30.
doi: 10.1213/01.ane.0000068801.28430.ed pmid: 12818971 |
| 14 |
Ilieva I, Ohgami K, Jin XH, Suzuki Y, Shiratori K, Yoshida K, et al. Captopril suppresses inflammation in endotoxin-induced uveitis in rats. Exp Eye Res. 2006; 83(3):651-7.
doi: 10.1016/j.exer.2006.03.005 |
| 15 |
Mizera R, Hodyc D, Herget J. ROS scavenger decreases basal perfusion pressure, vasoconstriction and NO synthase activity in pulmonary circulation during pulmonary microembolism. Physiol Res. 2015; 64(5):683-8.
pmid: 25804094 |
| 16 |
Tuder RM, Stacher E, Robinson J, Kumar R, Graham BB. Pathology of pulmonary hypertension. Clin Chest Med. 2013; 34(4):639-50.
doi: 10.1016/j.ccm.2013.08.009 |
| 17 |
Kugathasan L, Ray JB, Deng YP, Rezaei E, Dumont DJ, Stewart DJ. The angiopietin-1-Tie2 pathway prevents rather than promotes pulmonary arterial hypertension in transgenic mice. J Exp Med. 2009; 206(10):2221-34.
doi: 10.1084/jem.20090389 |
| 18 |
Kümpers P, Nickel N, Lukasz A, Golpon H, Westerkamp V, Olsson KM, et al. Circulating angiopoietins in idiopathic pulmonary arterial hypertension. Eur Heart J. 2010; 31(18):2291-300.
doi: 10.1093/eurheartj/ehq226 |
| 19 | Lüscher TF. Endothelial dysfunction: the role and impact of the renin-angiotensin system. Heart. 2000;84 Suppl 1 (Suppl 1): i20-2: discussion i50. |
| 20 |
Ferreira AJ, Shenoy V, Yamazato Y, Sriramula S, Francis J, Yuan L, et al. Evidence for angiotensin-converting enzyme 2 as a therapeutic target for the prevention of pulmonary hypertension. Am J Respir Crit Care Med. 2009; 179(11):1048-54.
doi: 10.1164/rccm.200811-1678OC |
| 21 |
Li G, Liu YL, Zhu YB, Liu AJ, Xu YL, Li XF, et al. ACE2 activation confers endothelial protection and attenuates neointimal lesions in prevention of severe pulmonary arterial hypertension in rats. Lung. 2013; 191(4):327-36.
doi: 10.1007/s00408-013-9470-8 |
| 22 |
Otani A, Takagi H, Oh H, Koyama S, Honda Y. Angiotensin II induces expression of the Tie2 receptor ligand, angiopoietin-2, in bovine retinal endothelial cells. Diabetes. 2001; 50(4):867-75.
doi: 10.2337/diabetes.50.4.867 pmid: 11289054 |
| 23 |
Madsen K, Marcussen N, Pedersen M, Kjaersgaard G, Facemire C, Coffman TM, et al. Angiotensin II promotes development of the renal microcirculation through AT1 receptorsv. J Am Soc Nephrol. 2010; 21(3):448-59.
doi: 10.1681/ASN.2009010045 |
| 24 |
Rizkalla B, Forbes JM, Cao Z, Boner G, Cooper ME. Temporal renal expression of angiogenic growth factors and their receptors in experimental diabetes: role of therenin-angiotensin system. J Hypertens. 2005; 23(1):153-64.
pmid: 15643138 |
| [1] | Chao-yu Lei, Heng-wei Qin, Xue-jie Dong, Jia-lin You, Lin Zhang. Layperson’s performance on an unconversant type of AED device: A prospective crossover simulation experimental study [J]. World Journal of Emergency Medicine, 2022, 13(2): 98-105. |
| [2] | Ji-yang Ling, Chun-sheng Li, Yun Zhang, Xiao-li Yuan, Bo Liu, Yong Liang, Qiang Zhang. Protective effect of extracorporeal membrane pulmonary oxygenation combined with cardiopulmonary resuscitation on post-resuscitation lung injury [J]. World Journal of Emergency Medicine, 2021, 12(4): 303-308. |
| [3] | Wei-jing Shao, Ting-ting Shu, Shuang Xu, Li-cai Liang, Jehane Michael Le Grange, Yu-ran Zhou, He Huang, Yu Cai, Qing Zhang, Peng Sun. Left-sided vagus nerve stimulation improves cardiopulmonary resuscitation outcomes in rats as effectively as right-sided vagus nerve stimulation [J]. World Journal of Emergency Medicine, 2021, 12(4): 309-316. |
| [4] | Xue-jie Dong, Lin Zhang, Yue-lin Yu, Shu-xiao Shi, Xiao-chen Yang, Xiao-qian Zhang, Shuang Tian, Helge Myklebust, Guo-hong Li, Zhi-jie Zheng. The general public’s ability to operate automated external defibrillator: A controlled simulation study [J]. World Journal of Emergency Medicine, 2020, 11(4): 238-245. |
| [5] | Ye-cheng Liu, Yan-meng Qi, Hui Zhang, Joseph Walline, Hua-dong Zhu. A survey of ventilation strategies during cardiopulmonary resuscitation [J]. World Journal of Emergency Medicine, 2019, 10(4): 222-227. |
| [6] | Alexei Birkun, Yekaterina Kosova. Social attitude and willingness to attend cardiopulmonary resuscitation training and perform resuscitation in the Crimea [J]. World Journal of Emergency Medicine, 2018, 9(4): 237-248. |
| [7] | Alexei Birkun, Maksim Glotov, Herman Franklin Ndjamen, Esther Alaiye, Temidara Adeleke, Sergey Samarin. Pre-recorded instructional audio vs. dispatchers’ conversational assistance in telephone cardiopulmonary resuscitation: A randomized controlled simulation study [J]. World Journal of Emergency Medicine, 2018, 9(3): 165-171. |
| [8] | Alexei Birkun, Maksim Glotov. Education in cardiopulmonary resuscitation in Russia: A systematic review of the available evidence [J]. World Journal of Emergency Medicine, 2017, 8(4): 245-252. |
| [9] | Chennappa Kalvatala Krishna, Hakim Irfan Showkat, Meenakshi Taktani, Vikram Khatri. Out of hospital cardiac arrest resuscitation outcome in North India — CARO study [J]. World Journal of Emergency Medicine, 2017, 8(3): 200-205. |
| [10] | Ji Ung Na, Sang Kuk Han, Pil Cho Choi, Dong Hyuk Shin. Effect of metronome rates on the quality of bag-mask ventilation during metronome-guided 30:2 cardiopulmonary resuscitation: A randomized simulation study [J]. World Journal of Emergency Medicine, 2017, 8(2): 136-140. |
| [11] | Gan-nan Wang, Xu-feng Chen, Li Qiao, Yong Mei, Jin-ru Lv, Xi-hua Huang, Bin Shen, Jin-song Zhang. Comparison of extracorporeal and conventional cardiopulmonary resuscitation: A meta-analysis of 2 260 patients with cardiac arrest [J]. World Journal of Emergency Medicine, 2017, 8(1): 5-11. |
| [12] | Marion Leary, David G. Buckler, Daniel J. Ikeda, Daiane A. Saraiva, Robert A. Berg, Vinay M. Nadkarni, Audrey L. Blewer, Benjamin S. Abella. The association of layperson characteristics with the quality of simulated cardiopulmonary resuscitation performance [J]. World Journal of Emergency Medicine, 2017, 8(1): 12-18. |
| [13] | Chik Leung Ho, Ka Wai Cheng, Tze Hang Ma, Yau Hang Wong, Ka Lok Cheng, Chak Wah Kam. Characterization of available automated external defibrillators in the market based on the product manuals in 2014 [J]. World Journal of Emergency Medicine, 2016, 7(2): 138-146. |
| [14] | Audrey L. Blewer, David G. Buckler, Jiaqi Li, Marion Leary, Lance B. Becker, Judy A. Shea, Peter W. Groeneveld, Mary E. Putt, Benjamin S. Abella. Impact of the 2010 resuscitation guidelines training on layperson chest compressions [J]. World Journal of Emergency Medicine, 2015, 6(4): 270-276. |
| [15] | Jian-ping Gao, Ke-jing Ying. Thrombolysis during extended cardiopulmonary resuscitation for autoimmune-related pulmonary embolism [J]. World Journal of Emergency Medicine, 2015, 6(2): 153-156. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||
