World Journal of Emergency Medicine ›› 2020, Vol. 11 ›› Issue (4): 238-245.doi: 10.5847/wjem.j.1920-8642.2020.04.006
Special Issue: Cardiopulmonary Resuscitation
• Original Article • Previous Articles Next Articles
Xue-jie Dong1, Lin Zhang1( ), Yue-lin Yu1, Shu-xiao Shi1, Xiao-chen Yang1, Xiao-qian Zhang2, Shuang Tian2, Helge Myklebust3, Guo-hong Li1, Zhi-jie Zheng4
), Yue-lin Yu1, Shu-xiao Shi1, Xiao-chen Yang1, Xiao-qian Zhang2, Shuang Tian2, Helge Myklebust3, Guo-hong Li1, Zhi-jie Zheng4
Received:2020-01-12
Accepted:2020-06-01
Online:2020-10-01
Published:2020-10-01
Contact:
Lin Zhang
E-mail:zhanglynn@sjtu.edu.cn
Xue-jie Dong, Lin Zhang, Yue-lin Yu, Shu-xiao Shi, Xiao-chen Yang, Xiao-qian Zhang, Shuang Tian, Helge Myklebust, Guo-hong Li, Zhi-jie Zheng. The general public’s ability to operate automated external defibrillator: A controlled simulation study[J]. World Journal of Emergency Medicine, 2020, 11(4): 238-245.
Add to citation manager EndNote|Ris|BibTeX
URL: http://wjem.com.cn//EN/10.5847/wjem.j.1920-8642.2020.04.006
Table 1
Assessment of correct critical actions in the general public aged 18-65 years, n (%)
| Critical actions | Pre-training (n=94) | Post-training (n=94) | Three-month follow-upa (n=82) | P-valueb (pre-training vs. post-training) | P-valueb (post-training vs. follow-up) |
|---|---|---|---|---|---|
| Successful defibrillations | 14 (14.9) | 66 (70.2) | 41 (50.0) | <0.001 | 0.01 |
| Turning on the AED | 94 (100.0) | 94 (100.0) | 82 (100.0) | - | - |
| Baring the chest | 59 (62.8) | 94 (100.0) | 75 (91.4) | <0.001 | 0.01 |
| Placing the electrodes | 66 (70.2) | 94 (100.0) | 78 (95.1) | <0.001 | 0.05 |
| Correct electrode placement | 17 (18.1) | 72 (76.6) | 44 (53.7) | <0.001 | <0.01 |
| Attaching the connector | 94 (100.0) | 94 (100.0) | 82 (100.0) | - | - |
| Clear while AED analyzes the rhythm | 72 (76.6) | 86 (91.5) | 76 (92.7) | 0.005 | 0.79 |
| Clear while AED delivers the shock | 87 (92.6) | 93 (98.9) | 79 (96.3) | 0.070 | 0.34 |
| Pressing the shock button | 94 (100.0) | 94 (100.0) | 82 (100.0) | - | - |
| Resuming CPR after shock | 9 (9.6) | 82 (87.2) | 46 (56.1) | <0.001 | <0.01 |
Table 2
Proportion of successful defibrillations and correct critical actions by age groups (years) and three skill assessment phases, n (%)
| Critical actions | Pre-training | Post-training | Three-month follow-upa | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 18-24 (n=32) | 25-54 (n=34) | 55-65 (n=28) | P-valueb | 18-24 (n=32) | 25-54 (n=34) | 55-65 (n=28) | P-valueb | 18-24 (n=31) | 25-54 (n=28) | 55-65 (n=23) | P-valueb | |
| Successful defibrillations | 8 (25.0) | 4 (11.8) | 2 (7.1) | 0.15 | 23 (71.9) | 24 (70.6) | 19 (67.9) | 0.96 | 17 (54.8) | 18 (64.3) | 6 (26.1) | 0.02 |
| Turning on the AED | 32 (100.0) | 34 (100.0) | 28 (100.0) | - | 32 (100.0) | 34 (100.0) | 28 (100.0) | - | 31 (100.0) | 28 (100.0) | 23 (100.0) | - |
| Baring the chest | 27 (84.4) | 25 (73.5) | 7 (25.0) | <0.01 | 32 (100.0) | 34 (100.0) | 28 (100.0) | - | 30 (96.8) | 26 (92.9) | 19 (82.6) | 0.37 |
| Placing the electrodes | 31 (96.9) | 26 (76.5) | 9 (32.1) | <0.01 | 32 (100.0) | 34 (100.0) | 28 (100.0) | - | 31 (100.0) | 27 (96.4) | 20 (87.0) | 0.06 |
| Correct electrode placement | 10 (31.3) | 4 (11.8) | 3 (10.7) | 0.06 | 27 (84.4) | 24 (70.6) | 21 (75.0) | 0.41 | 17 (54.8) | 18 (64.3) | 6 (26.1) | 0.02 |
| Attaching the connectors | 32 (100.0) | 34 (100.0) | 28 (100.0) | - | 32 (100.0) | 34 (100.0) | 28 (100.0) | - | 31 (100.0) | 28 (100.0) | 23 (100.0) | - |
| Clear while AED analyzes the rhythm | 27 (84.4) | 27 (79.4) | 18 (64.3) | 0.17 | 27 (84.4) | 33 (97.1) | 26 (92.9) | 0.18 | 28 (90.3) | 28 (100.0) | 20 (87.0) | 0.17 |
| Clear while AED delivers the shock | 31 (96.9) | 34 (100.0) | 22 (78.6) | 0.01 | 31 (96.9) | 34 (100.0) | 28 (100.0) | 0.38 | 28 (90.3) | 28 (100.0) | 23 (100.0) | 0.11 |
| Pressing the shock button | 32 (100.0) | 34 (100.0) | 28 (100.0) | - | 32 (100.0) | 34 (100.0) | 28 (100.0) | - | 31 (100.0) | 28 (100.0) | 23 (100.0) | - |
| Resuming CPR after shock | 3 (9.4) | 4 (11.8) | 2 (7.1) | 0.91 | 26 (81.3) | 30 (88.2) | 26 (92.9) | 0.43 | 22 (71.0) | 20 (71.4) | 4 (17.4) | <0.01 |

Figure 2.
Assessment of AED electrode placement in the study participants by age group. The star icons represented the standard electrode positions that were placed according to the AED’s instructional diagrams. Placement of AED electrode by participants within 5 cm of this standard was defined as correct. The coordinates (10, 0) and (-10, 0) represented the manikin’s left and right nipples, respectively.
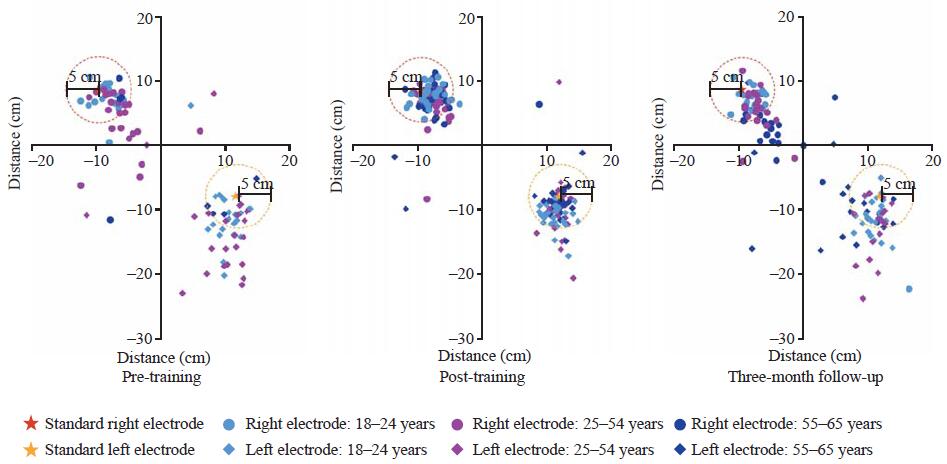

Figure 3.
Timelines of successful defibrillations by the general public aged 18-65 years. t1: start of baring chest; t2: AED power on; t3: start of attaching electrodes; t4: start of inserting the plug; t5: AED indicating a shock; t6: delivering the shock; and t7: resuming CPR. Median values are shown (interquartile range). P-values were derived using the Mann-Whitney U-test. A P-value <0.05 was considered statistically significant.
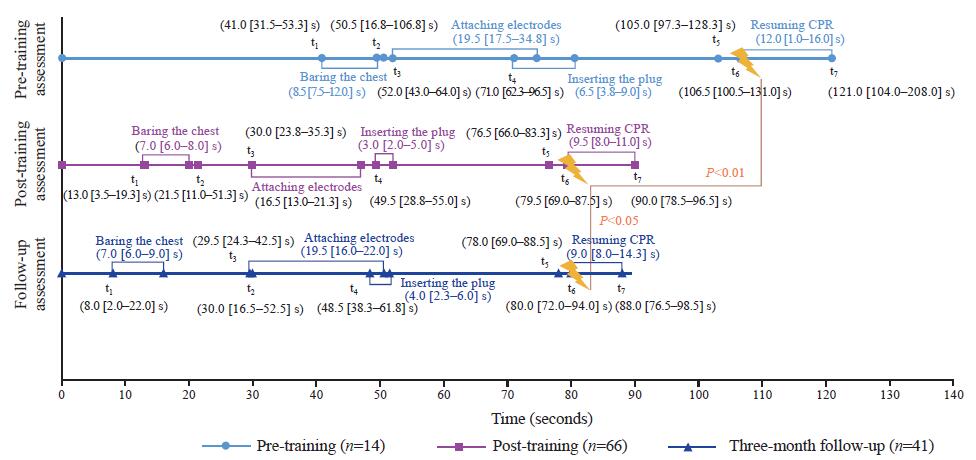
Table 3
Comparison of time intervals in successful defibrillations by age groups (years) and three skill assessment phases, seconds, M (P25-P75) a
| Time intervals | Pre-training | Post-training | Three-month follow-up | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 18-24 (n=8) | 25-54 (n=4) | 55-65 (n=2)b | P-valuec | 18-24 (n=23) | 25-54 (n=24) | 55-65 (n=19) | P-valuec | 18-24 (n=17) | 25-54 (n=18) | 55-65 (n=6) | P-valuec | |
| Time for power on | 79 (20-155) | 28 (13-92) | 18, 39 | 0.06 | 26 (11-52) | 17 (10-43) | 20 (12-56) | 0.38 | 31 (22-53) | 29 (17-52) | 32 (9-41) | 0.07 |
| Time to start baring chest | 42 (31-65) | 44 (41-51) | 1, 19 | 0.55 | 12 (4-17) | 16 (6-25) | 14 (1-22) | 0.48 | 4 (1-11) | 9 (3-24) | 15 (10-31) | 0.14 |
| Time for baring the chest | 12 (8-15) | 8 (7-10) | 4, 5 | 0.08 | 7 (6-8) | 7 (6-9) | 6 (6-7) | 0.54 | 6 (6-10) | 8 (6-10) | 8 (7-8) | 0.78 |
| Time for placing the electrodes | 24 (18-36) | 23 (17-45) | 14, 17 | 0.03 | 16 (13-23) | 17 (11-23) | 16 (13-19) | 0.60 | 20 (18-22) | 19 (14-23) | 16 (13-18) | 0.02 |
| Time for inserting the plug | 8 (4-11) | 6 (3-8) | 5, 7 | 0.94 | 4 (2-4) | 3 (2-6) | 3 (3-5) | 0.10 | 4 (3-7) | 3 (2-5) | 6 (4-6) | 0.41 |
| Time for AED indicating a shock | 113 (99-177) | 105 (100-125) | 81, 88 | 0.09 | 73 (62-83) | 79 (66-86) | 76 (72-82) | 0.96 | 78 (73-87) | 74 (63-90) | 86 (72-103) | 0.33 |
| Time for response to shock instruction | 3 (3-4) | 5 (3-5) | 4, 4 | 0.31 | 2 (1-3) | 3 (2-4) | 3 (2-4) | 0.01 | 4 (2-4) | 4 (2-5) | 5 (3-6) | 0.56 |
| Time for shock | 117 (102-181) | 110 (105-128) | 85, 92 | 0.09 | 76 (63-86) | 82 (69-91) | 79 (77-86) | 0.90 | 80 (76-90) | 78 (68-95) | 93 (75-106) | 0.38 |
| Time for resuming CPR after shock | 6 (1-12) | 15 (12-15) | 16, 16 | 0.23 | 9 (6-10) | 9 (8-10) | 10 (9-12) | 0.01 | 12.5 (6-20) | 9 (8-11) | 9 (9-9) | 0.16 |
| 1 |
Kleinman ME, Brennan EE, Goldberger ZD, Swor RA, Terry M, Bobrow BJ, et al. Part 5: Adult Basic Life Support and Cardiopulmonary Resuscitation Quality: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2015; 132(18 Suppl 2):S414-35.
doi: 10.1161/CIR.0000000000000259 pmid: 26472993 |
| 2 |
Perkins GD, Handley AJ, Koster RW, Castren M, Smyth MA, Olasveengen T, et al. European Resuscitation Council Guidelines for Resuscitation 2015: Section 2. Adult Basic Life Support and Automated External Defibrillation. Resuscitation. 2015; 95:81-99.
doi: 10.1016/j.resuscitation.2015.07.015 pmid: 26477420 |
| 3 |
Baekgaard JS, Viereck S, Moller TP, Ersboll AK, Lippert F, Folke F. The effects of public access defibrillation on survival after out-of-hospital cardiac arrest: a systematic review of observational studies. Circulation. 2017; 136(10):954-65.
doi: 10.1161/CIRCULATIONAHA.117.029067 pmid: 28687709 |
| 4 |
Holmberg MJ, Vognsen M, Andersen MS, Donnino MW, Andersen LW. Bystander automated external defibrillator use and clinical outcomes after out-of-hospital cardiac arrest: a systematic review and meta-analysis. Resuscitation. 2017; 120:77-87.
doi: 10.1016/j.resuscitation.2017.09.003 pmid: 28888810 |
| 5 |
Sasson C, Rogers MAM, Dahl J, Kellermann AL. Predictors of survival from out-of-hospital cardiac arrest: a systematic review and meta-analysis. Circ Cardiovasc Qual Outcomes. 2010; 3(1):63-81.
doi: 10.1161/CIRCOUTCOMES.109.889576 pmid: 20123673 |
| 6 |
Kiyohara K, Kitamura T, Sakai T, Nishiyama C, Nishiuchi T, Hayashi Y, et al. Public-access AED pad application and outcomes for out-of-hospital cardiac arrests in Osaka, Japan. Resuscitation. 2016; 106:70-5.
doi: 10.1016/j.resuscitation.2016.06.025 pmid: 27373223 |
| 7 |
Zijlstra JA, Bekkers LE, Hulleman M, Beesems SG, Koster RW. Automated external defibrillator and operator performance in out-of-hospital cardiac arrest. Resuscitation. 2017; 118:140-6.
doi: 10.1016/j.resuscitation.2017.05.017 pmid: 28526495 |
| 8 |
Bodtker H, Rosendahl D. Automated external defibrillators and defibrillation electrodes from major manufactures depict placement of the left apical defibrillation electrode poorly! Resuscitation. 2018; 125:e11-e2.
doi: 10.1016/j.resuscitation.2018.01.046 pmid: 29408601 |
| 9 |
Agerskov M, Nielsen AM, Hansen CM, Hansen MB, Lippert FK, Wissenberg M, et al. Public access defibrillation: great benefit and potential but infrequently used. Resuscitation. 2015; 96:53-8.
doi: 10.1016/j.resuscitation.2015.07.021 pmid: 26234893 |
| 10 |
Olasveengen TM, de Caen AR, Mancini ME, Maconochie IK, Aickin R, Atkins DL, et al. 2017 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science with Treatment Recommendations Summary. Resuscitation. 2017; 121:201-14.
doi: 10.1016/j.resuscitation.2017.10.021 pmid: 29128145 |
| 11 |
Yeung J, Okamoto D, Soar J, Perkins GD. AED training and its impact on skill acquisition, retention and performance—a systematic review of alternative training methods. Resuscitation. 2011; 82(6):657-64.
doi: 10.1016/j.resuscitation.2011.02.035 |
| 12 |
Gundry JW, Comess KA, DeRook FA, Jorgenson D, Bardy GH, . Comparison of naive sixth-grade children with trained professionals in the use of an automated external defibrillator. Circulation. 1999; 100(16):1703-7.
doi: 10.1161/01.cir.100.16.1703 pmid: 10525489 |
| 13 |
Beckers S, Fries M, Bickenbach J, Derwall M, Kuhlen R, Rossaint R. Minimal instructions improve the performance of laypersons in the use of semiautomatic and automatic external defibrillators. Crit Care. 2005; 9(2):R110-6.
doi: 10.1186/cc3033 pmid: 15774042 |
| 14 |
Beckers SK, Fries M, Bickenbach J, Skorning MH, Derwall M, Kuhlen R, et al. Retention of skills in medical students following minimal theoretical instructions on semi and fully automated external defibrillators. Resuscitation. 2007; 72(3):444-50.
doi: 10.1016/j.resuscitation.2006.08.001 pmid: 17188417 |
| 15 |
Mattei LC, McKay U, Lepper MW, Soar J. Do nurses and physiotherapists require training to use an automated external defibrillator? Resuscitation. 2002; 53(3):277-80.
doi: 10.1016/s0300-9572(02)00023-0 pmid: 12062843 |
| 16 |
Wissenberg M, Lippert FK, Folke F, Weeke P, Hansen CM, Christensen EF, et al. Association of national initiatives to improve cardiac arrest management with rates of bystander intervention and patient survival after out-of-hospital cardiac arrest. JAMA. 2013; 310(13):1377-84.
doi: 10.1001/jama.2013.278483 pmid: 24084923 |
| 17 | Global Resuscitation Alliance. The WeCan CPR Training Program in China. Available at https://www.globalresuscitationalliance.org/wp-content/uploads/2019/12/China_Community_Training.pdf. July 20, 2020 update. |
| 18 |
Soar J, Nolan JP, Bottiger BW, Perkins GD, Lott C, Carli P, et al. European Resuscitation Council Guidelines for Resuscitation 2015: Section 3. Adult Advanced Life Support. Resuscitation. 2015; 95:100-47.
doi: 10.1016/j.resuscitation.2015.07.016 pmid: 26477701 |
| 19 |
Smith CM, Lim Choi Keung SN, Khan MO, Arvanitis TN, Fothergill R, Hartley-Sharpe C, et al. Barriers and facilitators to public access defibrillation in out-of-hospital cardiac arrest: a systematic review. Eur Heart J Qual Care Clin Outcomes. 2017; 3(4):264-73.
doi: 10.1093/ehjqcco/qcx023 pmid: 29044399 |
| 20 |
Smith CM, Perkins GD. Improving bystander defibrillation for out-of-hospital cardiac arrest: capability, opportunity and motivation. Resuscitation. 2018; 124:A15-6.
doi: 10.1016/j.resuscitation.2018.01.006 pmid: 29337173 |
| 21 |
Zhang L, Li B, Zhao X, Zhang Y, Deng Y, Zhao A, et al. Public access of automated external defibrillators in a metropolitan city of China. Resuscitation. 2019; 140:120-6.
doi: 10.1016/j.resuscitation.2019.05.015 pmid: 31129230 |
| 22 |
Basanta Camiño S, Navarro Patón R, Freire Tellado M, Barcala Furelos R, Pavón Prieto MP, Fernández López M, et al. Assessment of knowledge and skills in using an automated external defibrillator (AED) by university students. A quasi-experimental study. Med Intensiva. 2017; 41(5):270-6.
doi: 10.1016/j.medin.2016.07.008 pmid: 27773493 |
| 23 |
Brooks B, Chan S, Lander P, Adamson R, Hodgetts GA, Deakin CD. Public knowledge and confidence in the use of public access defibrillation. Heart. 2015; 101(12):967-71.
doi: 10.1136/heartjnl-2015-307624 pmid: 25926599 |
| 24 |
Esibov A, Chapman FW, Melnick SB, Sullivan JL, Walcott GP. Minor variations in electrode pad placement impact defibrillation success. Prehosp Emerg Care. 2016; 20(2):292-8.
doi: 10.3109/10903127.2015.1076095 pmid: 26383036 |
| 25 |
Staerk M, Bodtker H, Lauridsen KG, Lofgren B. Automated external defibrillation training on the left or the right side—a randomized simulation study. Open Access Emerg Med. 2017; 9:73-9.
doi: 10.2147/OAEM.S140220 pmid: 29066936 |
| 26 |
Bodtker H, Rosendahl D. Correct AED electrode placement is rarely achieved by laypersons when attaching AED electrodes to a human thorax. Resuscitation. 2018; 127:e12-3.
doi: 10.1016/j.resuscitation.2018.04.002 pmid: 29627397 |
| 27 |
Nurmi J, Castren M. Layperson positioning of defibrillation electrodes guided by pictorial instructions. Resuscitation. 2005; 64(2):177-80.
doi: 10.1016/j.resuscitation.2004.08.014 pmid: 15680526 |
| 28 |
Foster AG, Deakin CD. Accuracy of instructional diagrams for automated external defibrillator pad positioning. Resuscitation. 2019; 139:282-8.
doi: 10.1016/j.resuscitation.2019.04.034 pmid: 31063839 |
| 29 |
Mosesso VN Jr, Shapiro AH, Stein K, Burkett K, Wang H. Effects of AED device features on performance by untrained laypersons. Resuscitation. 2009; 80(11):1285-9.
doi: 10.1016/j.resuscitation.2009.07.016 |
| 30 |
Greif R, Lockey AS, Conaghan P, Lippert A, De Vries W, Monsieurs KG, et al. European Resuscitation Council Guidelines for Resuscitation 2015: Section 10. Education and implementation of resuscitation. Resuscitation. 2015; 95:288-301.
doi: 10.1016/j.resuscitation.2015.07.032 pmid: 26477418 |
| 31 |
Bhanji F, Donoghue AJ, Wolff MS, Flores GE, Halamek LP, Berman JM, et al. Part 14: Education: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2015; 132(18 suppl 2):S561-73.
doi: 10.1161/CIR.0000000000000268 pmid: 26473002 |
| 32 |
Meischke HW, Rea T, Eisenberg MS, Schaeffer SM, Kudenchuk P. Training seniors in the operation of an automated external defibrillator: a randomized trial comparing two training methods. Ann Emerg Med. 2001; 38(3):216-22.
doi: 10.1067/mem.2001.115621 |
| 33 |
Mitchell KB, Gugerty L, Muth E. Effects of brief training on use of automated external defibrillators by people without medical expertise. Hum Factors. 2008; 50(2):301-10.
doi: 10.1518/001872008X250746 pmid: 18516840 |
| 34 |
Christenson J, Nafziger S, Compton S, Vijayaraghavan K, Slater B, Ledingham R, et al. The effect of time on CPR and automated external defibrillator skills in the public access defibrillation trial. Resuscitation. 2007; 74(1):52-62.
doi: 10.1016/j.resuscitation.2006.11.005 pmid: 17303309 |
| 35 |
Woollard M, Whitfield R, Newcombe RG, Colquhoun M, Vetter N, Chamberlain D. Optimal refresher training intervals for AED and CPR skills: a randomised controlled trial. Resuscitation. 2006; 71(2):237-47.
doi: 10.1016/j.resuscitation.2006.04.005 pmid: 17010497 |
| 36 | Mabrouk Z, Helmert JR, Müller MP. Evaluation of a usability optimized AED design. Resuscitation. 2018; 130:e57-8. |
| 37 |
Maes F, Marchandise S, Boileau L, Le Polain de Waroux JB, Scavee C. Evaluation of a new semiautomated external defibrillator technology: a live case video recording study. Emerg Med J. 2015; 32(6):481-5.
doi: 10.1136/emermed-2013-202962 pmid: 25082717 |
| 38 |
Carballo-Fazanes A, Jorge-Soto C, Abelairas-Gómez C, Bello-Rodríguez J, Fernández-Méndez F, Rodríguez-Núñez A. Could mobile apps improve laypeople AED use? Resuscitation. 2019; 140:159-60.
doi: 10.1016/j.resuscitation.2019.05.029 pmid: 31153946 |
| [1] | Janett Kreutziger, Philip Puchner, Stefan Schmid, Wolfgang Mayer, Harald Prossliner, Wolfgang Lederer. Accuracy of training blood volume quantification using a visual estimation tool [J]. World Journal of Emergency Medicine, 2021, 12(3): 174-178. |
| [2] | Alexei Birkun, Fatima Trunkwala, Adhish Gautam, Miriam Okoroanyanwu, Adesokan Oyewumi. Availability of basic life support courses for the general populations in India, Nigeria and the United Kingdom: An internet-based analysis [J]. World Journal of Emergency Medicine, 2020, 11(3): 133-139. |
| [3] | Avir Mitra, Asaf Gave, Kelsey Coolahan, Thomas Nguyen. Confirmation of endotracheal tube placement using disposable fiberoptic bronchoscopy in the emergent setting [J]. World Journal of Emergency Medicine, 2019, 10(4): 210-214. |
| [4] | Ye-cheng Liu, Yan-meng Qi, Hui Zhang, Joseph Walline, Hua-dong Zhu. A survey of ventilation strategies during cardiopulmonary resuscitation [J]. World Journal of Emergency Medicine, 2019, 10(4): 222-227. |
| [5] | Alexander S. Kwon, Shadi Lahham, John C. Fox. Can an 8th grade student learn point of care ultrasound? [J]. World Journal of Emergency Medicine, 2019, 10(2): 109-113. |
| [6] | Alexei Birkun, Yekaterina Kosova. Social attitude and willingness to attend cardiopulmonary resuscitation training and perform resuscitation in the Crimea [J]. World Journal of Emergency Medicine, 2018, 9(4): 237-248. |
| [7] | Michael D.T. Yue, David W. Spivey, Daniel B. Gingold, Douglas G. Sward. The effect of wilderness and medical training on injury and altitude preparedness among backcountry hikers in Rocky Mountain National Park [J]. World Journal of Emergency Medicine, 2018, 9(3): 172-177. |
| [8] | Alexei Birkun, Maksim Glotov, Herman Franklin Ndjamen, Esther Alaiye, Temidara Adeleke, Sergey Samarin. Pre-recorded instructional audio vs. dispatchers’ conversational assistance in telephone cardiopulmonary resuscitation: A randomized controlled simulation study [J]. World Journal of Emergency Medicine, 2018, 9(3): 165-171. |
| [9] | Ahmad Aalam, Mark Zocchi, Khalid Alyami, Abdullah Shalabi, Abdullah Bakhsh, Asaad Alsufyani, Abdulrahman Sabbagh, Mohammed Alshahrani, Jesse M. Pines. Perceptions of emergency medicine residents on the quality of residency training in the United States and Saudi Arabia [J]. World Journal of Emergency Medicine, 2018, 9(1): 5-13. |
| [10] | Alexei Birkun, Maksim Glotov. Education in cardiopulmonary resuscitation in Russia: A systematic review of the available evidence [J]. World Journal of Emergency Medicine, 2017, 8(4): 245-252. |
| [11] | Chennappa Kalvatala Krishna, Hakim Irfan Showkat, Meenakshi Taktani, Vikram Khatri. Out of hospital cardiac arrest resuscitation outcome in North India — CARO study [J]. World Journal of Emergency Medicine, 2017, 8(3): 200-205. |
| [12] | Ji Ung Na, Sang Kuk Han, Pil Cho Choi, Dong Hyuk Shin. Effect of metronome rates on the quality of bag-mask ventilation during metronome-guided 30:2 cardiopulmonary resuscitation: A randomized simulation study [J]. World Journal of Emergency Medicine, 2017, 8(2): 136-140. |
| [13] | Gan-nan Wang, Xu-feng Chen, Li Qiao, Yong Mei, Jin-ru Lv, Xi-hua Huang, Bin Shen, Jin-song Zhang. Comparison of extracorporeal and conventional cardiopulmonary resuscitation: A meta-analysis of 2 260 patients with cardiac arrest [J]. World Journal of Emergency Medicine, 2017, 8(1): 5-11. |
| [14] | Marion Leary, David G. Buckler, Daniel J. Ikeda, Daiane A. Saraiva, Robert A. Berg, Vinay M. Nadkarni, Audrey L. Blewer, Benjamin S. Abella. The association of layperson characteristics with the quality of simulated cardiopulmonary resuscitation performance [J]. World Journal of Emergency Medicine, 2017, 8(1): 12-18. |
| [15] | Mario Kobras, Sascha Langewand, Christina Murr, Christiane Neu, Jeannette Schmid. Short lessons in basic life support improve self-assurance in performing cardiopulmonary resuscitation [J]. World Journal of Emergency Medicine, 2016, 7(4): 255-262. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||
