World Journal of Emergency Medicine ›› 2024, Vol. 15 ›› Issue (3): 206-213.doi: 10.5847/wjem.j.1920-8642.2024.035
• Original Articles • Previous Articles Next Articles
A-ling Tang1,2, Yan Li1, Li-chao Sun1, Xiao-yu Liu1, Nan Gao1, Sheng-tao Yan1( ), Guo-qiang Zhang1(
), Guo-qiang Zhang1( )
)
Received:2023-12-20
Accepted:2024-03-16
Online:2024-05-15
Published:2024-05-01
Contact:
Guoqiang Zhang, Email: A-ling Tang, Yan Li, Li-chao Sun, Xiao-yu Liu, Nan Gao, Sheng-tao Yan, Guo-qiang Zhang. Xuebijing improves intestinal microcirculation dysfunction in septic rats by regulating the VEGF-A/PI3K/Akt signaling pathway[J]. World Journal of Emergency Medicine, 2024, 15(3): 206-213.
Add to citation manager EndNote|Ris|BibTeX
URL: http://wjem.com.cn/EN/10.5847/wjem.j.1920-8642.2024.035

Figure 1.
Effects of XBJ on sepsis-induced disruption of intestinal microcirculation dysfunction (sample size for each group=6). A: total vessel density (TVD); B: microvascular flow index 16 (MFI16); C: proportion of perfused vessels (PPV); D: perfusion vessel density (PVD). XBJ: Xuebijing; CLP: cecal ligation and puncture. Compared with the sham group, #P<0.05, ##P<0.01; compared with the CLP group, *P<0.05, **P<0.01; compared with the XBJ + axitinib group, ΔΔ P<0.01.
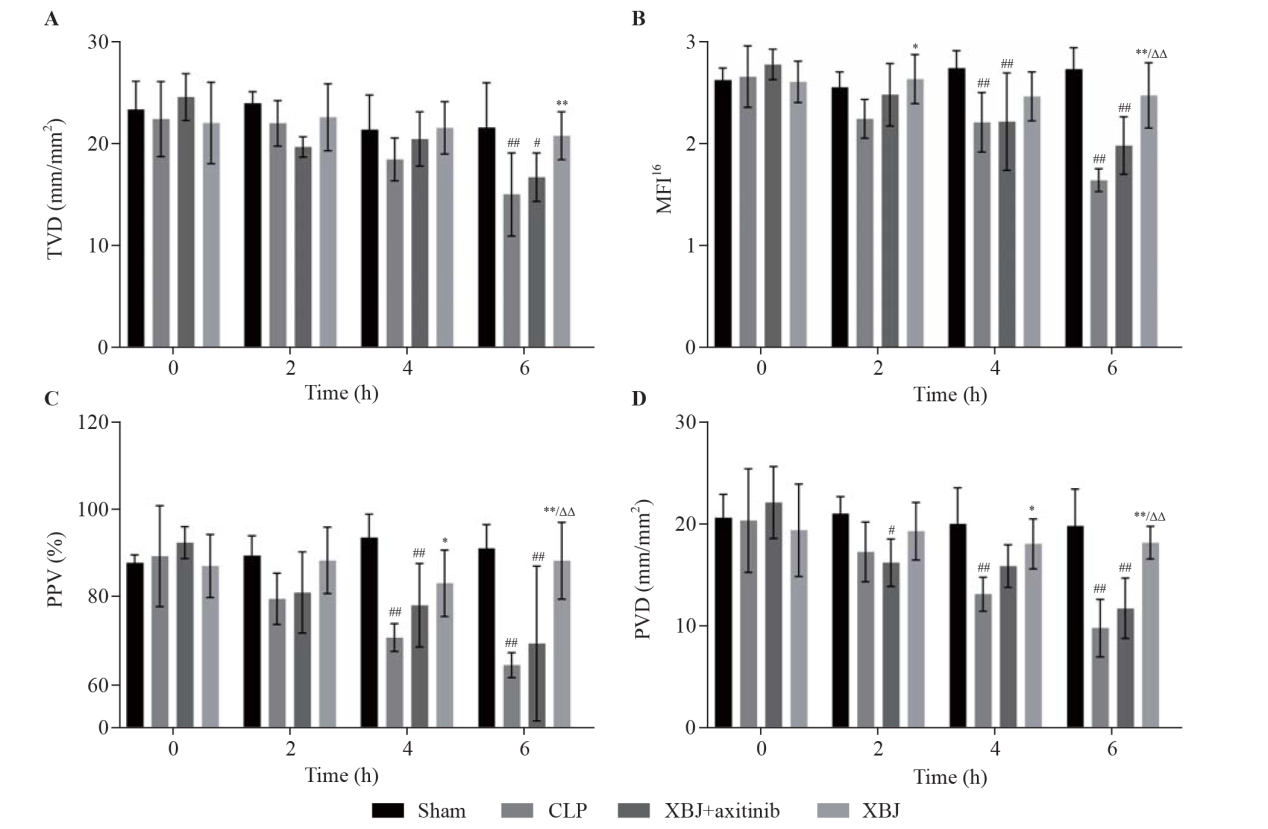
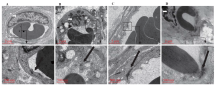
Figure 3.
Effect of XBJ on sepsis-induced destruction of small intestinal vascular endothelial cells. A: sham group (7,000×; 20,000×); B: CLP group (7,000×; 20,000×); C: XBJ + axitinib group (7,000×; 20,000×); D: XBJ group (7,000×; 20,000×). Triangular arrows: dense and chaotic cytoplasmic processes; long thick black arrows: tight junctions; short thick black arrows: mitochondrial edema and vacuolation; white arrows: deformed nuclei.

Figure 4.
Protein expression of PI3K/Akt in the rat small intestine (sample size for each group=3). A: Western blotting images of p-Akt, total Akt, p-PI3K, and total PI3K; B: p-PI3K/total PI3K; C: p-Akt/total Akt. XBJ: Xuebijing; CLP: cecal ligation and puncture; PI3K: phosphatidylinositol 3-kinase; Akt: protein kinase B; p-Akt: phosphorylated Akt; p-PI3K: phosphorylated PI3K. Compared with the CLP group, *P<0.05; compared with the XBJ + axitinib group, #P<0.05.
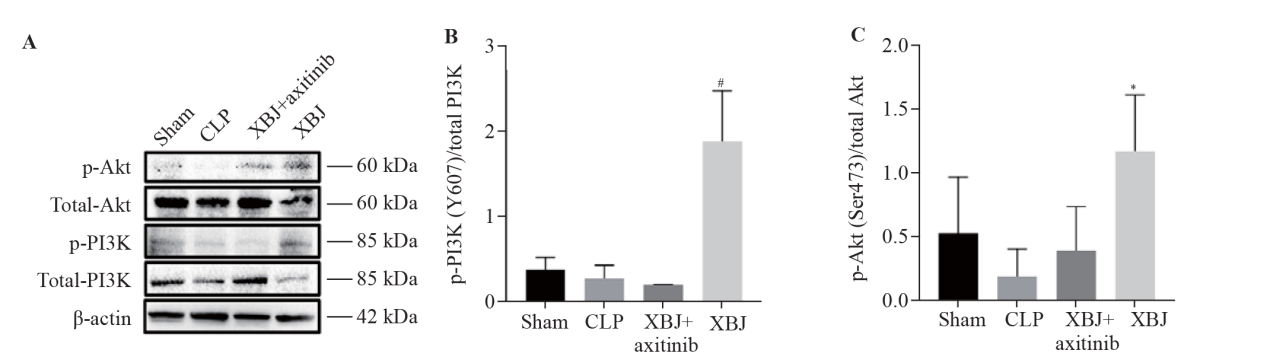

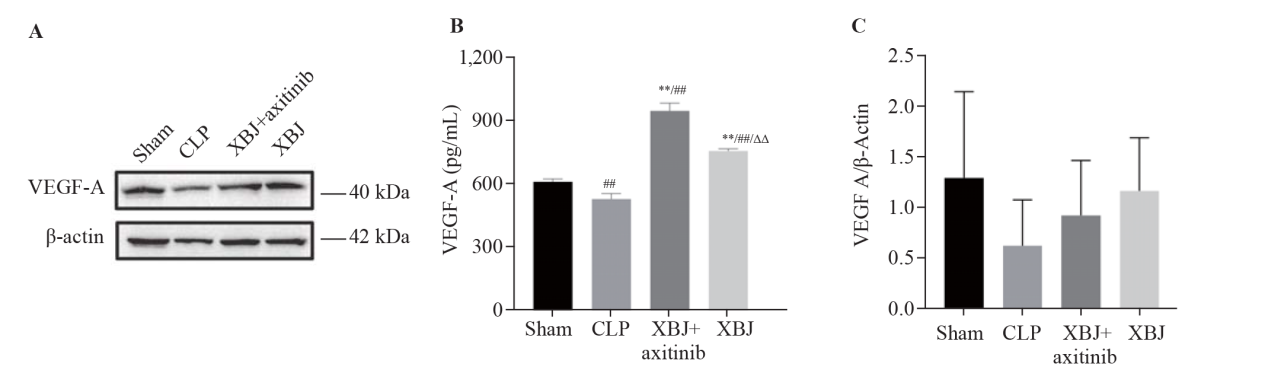
Figure 5.
Protein expression of VEGF-A in the rat small intestine. A: Western blotting images of VEGF-A (sample size for each group=3); B: ELISA results for VEGF-A (sample size for each group= 6); C: VEGF-A/β-actin (sample size for each group=3). XBJ: Xuebijing; CLP: cecal ligation and puncture; VEGF-A: vascular endothelial growth factor A; ELISA: enzyme-linked immunosorbent assay.
| 1 | Zhang WY, Chen ZH, An XX, Li H, Zhang HL, Wu SJ, et al. Analysis and validation of diagnostic biomarkers and immune cell infiltration characteristics in pediatric sepsis by integrating bioinformatics and machine learning. World J Pediatr. 2023; 19(11):1094-1103. |
| 2 | Wei JX, Jiang HL, Chen XH. Endothelial cell metabolism in sepsis. World J Emerg Med. 2023; 14(1):10-6. |
| 3 |
Lelubre C, Vincent JL. Mechanisms and treatment of organ failure in sepsis. Nat Rev Nephrol. 2018; 14(7):417-27.
doi: 10.1038/s41581-018-0005-7 pmid: 29691495 |
| 4 |
Tang AL, Shen MJ, Zhang GQ. Intestinal microcirculation dysfunction in sepsis: pathophysiology, clinical monitoring, and therapeutic interventions. World J Emerg Med. 2022; 13(5):343-8.
doi: 10.5847/wjem.j.1920-8642.2022.031 pmid: 36119779 |
| 5 | Heitrich M, García DM, Stoyanoff TR, Rodríguez JP, Todaro JS, Aguirre MV. Erythropoietin attenuates renal and pulmonary injury in polymicrobial induced-sepsis through EPO-R, VEGF and VEGF-R2 modulation. Biomed Pharmacother. 2016;82:606-13. |
| 6 | Thickett DR, Armstrong L, Millar AB. A role for vascular endothelial growth factor in acute and resolving lung injury. Am J Respir Crit Care Med. 2002; 166(10):1332-7. |
| 7 |
Abid MR, Guo SD, Minami T, Spokes KC, Ueki K, Skurk C, et al. Vascular endothelial growth factor activates PI3K/Akt/forkhead signaling in endothelial cells. Arterioscler Thromb Vasc Biol. 2004; 24(2):294-300.
doi: 10.1161/01.ATV.0000110502.10593.06 pmid: 14656735 |
| 8 | Jiang BH, Liu LZ. Akt signaling in regulating angiogenesis. Curr Cancer Drug Targets. 2008; 8(1):19-26. |
| 9 |
Sun Z, Zuo L, Sun T, Tang J, Ding D, Zhou L, et al. Chemical profiling and quantification of Xuebijing injection, a systematic quality control strategy using UHPLC-Q Exactive hybrid quadrupole-orbitrap high-resolution mass spectrometry. Sci Rep. 2017; 7(1):16921.
doi: 10.1038/s41598-017-17170-y pmid: 29208914 |
| 10 | Liu JF, Wang ZZ, Lin J, Li T, Guo XJ, Pang R, et al. Xuebijing injection in septic rats mitigates kidney injury, reduces cortical microcirculatory disorders, and suppresses activation of local inflammation. J Ethnopharmacol. 2021; 276:114199. |
| 11 | Huang ZY, Yang P. Effect of Xuebijing on intestinal microcirculation in septic rats. Proceedings of 17th Annual Congress of the Chinese Society for Emergency Medicine. 2014;109-10. (Article in Chinese) |
| 12 |
Rittirsch D, Huber-Lang MS, Flierl MA, Ward PA. Immunodesign of experimental sepsis by cecal ligation and puncture. Nat Protoc. 2009; 4(1):31-6.
doi: 10.1038/nprot.2008.214 pmid: 19131954 |
| 13 | Pancoto JAT, Corrêa PBF, Oliveira-Pelegrin GR, Rocha MJA. Autonomic dysfunction in experimental sepsis induced by cecal ligation and puncture. Auton Neurosci. 2008; 138(1-2):57-63. |
| 14 | Zhang QF, Gao ZJ, Zhang ZW, Zhao XG, Feng JK, Xu YF, et al. Impacts of high-voltage electrical burn on serum platelet-related factors and platelet aggregation number in rats and the interventive effect of Xuebijing. Zhonghua Shao Shang Za Zhi. 2020; 36(6):426-32. (Article in Chinese) |
| 15 |
Imai S, Miyake H, Fujisawa M. Acceleration of proteinuria without significant impact on renal function and its protection by angiotensin II receptor blocker in rats treated with axitinib. Target Oncol. 2016; 11(3):309-15.
doi: 10.1007/s11523-015-0393-6 pmid: 26423685 |
| 16 | Zhang L, Wang YX, Cao C, Zhu YK, Huang W, Yang Y, et al. Beneficial effect of Xuebijing against Pseudomonas aeruginosa infection in Caenorhabditis elegans. Front Pharmacol. 2022; 13: 949608. |
| 17 |
Thorburn T, Aali M, Kostek L, LeTourneau-Paci C, Colp P, Zhou J, et al. Anti-inflammatory effects of a novel iron chelator, DIBI, in experimental sepsis. Clin Hemorheol Microcirc. 2017; 67(3-4):241-50.
doi: 10.3233/CH-179205 pmid: 28869457 |
| 18 |
Dumbarton TC, Maxan A, Farah N, Sharawy N, Zhou J, Nantais J, et al. Tetrahydrobiopterin improves microcirculation in experimental sepsis. Clin Hemorheol Microcirc. 2017; 67(1):15-24.
doi: 10.3233/CH-160207 pmid: 28598830 |
| 19 |
Andersson A, Rundgren M, Kalman S, Rooyackers O, Brattstrom O, Oldner A, et al. Gut microcirculatory and mitochondrial effects of hyperdynamic endotoxaemic shock and norepinephrine treatment. Br J Anaesth. 2012; 108(2):254-61.
doi: 10.1093/bja/aer379 pmid: 22157851 |
| 20 |
Liu ZJ, Zeng ZH, Wu CD, Liu H. Tropisetron inhibits sepsis by repressing hyper-inflammation and regulating the cardiac action potential in rat models. Biomed Pharmacother. 2019; 110:380-8.
doi: S0753-3322(18)35470-2 pmid: 30529771 |
| 21 |
Li J, Olaleye OE, Yu X, Jia WW, Yang JL, Lu C, et al. High degree of pharmacokinetic compatibility exists between the five-herb medicine Xuebijing and antibiotics comedicated in sepsis care. Acta Pharm Sin B. 2019; 9(5):1035-49.
doi: 10.1016/j.apsb.2019.06.003 pmid: 31649852 |
| 22 | Yin Q, Li CS. Treatment effects of Xuebijing injection in severe septic patients with disseminated intravascular coagulation. Evid Based Complement Alternat Med. 2014; 2014:949254. |
| 23 | Liao XZ, Tao LT, Liu JH, Gu YY, Xie J, Chen YL, et al. Matrine combined with cisplatin synergistically inhibited urothelial bladder cancer cells via down-regulating VEGF/PI3K/Akt signaling pathway. Cancer Cell Int. 2017; 17:124. |
| 24 | Ruan GX, Kazlauskas A. VEGF-A engages at least three tyrosine kinases to activate PI3K/Akt. Cell Cycle. 2012; 11(11):2047-8. |
| 25 |
Sljivancanin Jakovljevic T, Martic J, Jacimovic J, Nikolic N, Milasin J, Mitrović TL. Association between innate immunity gene polymorphisms and neonatal sepsis development: a systematic review and meta-analysis. World J Pediatr. 2022; 18(10):654-70.
doi: 10.1007/s12519-022-00569-7 pmid: 35666457 |
| 26 | Sun P, Wei S, Wei X, Wang JQ, Zhang YY, Qiao MQ, et al. Anger emotional stress influences VEGF/VEGFR2 and its induced PI3K/Akt/mTOR signaling pathway. Neural Plast. 2016; 2016:4129015. |
| 27 |
Jesmin S, Zaedi S, Islam AM, Sultana SN, Iwashima Y, Wada T, et al. Time-dependent alterations of VEGF and its signaling molecules in acute lung injury in a rat model of sepsis. Inflammation. 2012; 35(2):484-500.
doi: 10.1007/s10753-011-9337-1 pmid: 21528367 |
| 28 | Zhou WA, Lai XX, Wang X, Yao XQ, Wang WH, Li S. Network pharmacology to explore the anti-inflammatory mechanism of Xuebijing in the treatment of sepsis. Phytomedicine. 2021; 85: 153543. |
| 29 | Zheng WJ, Yan Q, Ni YS, Zhan SF, Yang LL, Zhuang HF, et al. Examining the effector mechanisms of Xuebijing injection on COVID-19 based on network pharmacology. BioData Min. 2020; 13:17. |
| 30 | Han XY, Liu X, Zhao X, Wang XK, Sun YZ, Qu C, et al. Dapagliflozin ameliorates sepsis-induced heart injury by inhibiting cardiomyocyte apoptosis and electrical remodeling through the PI3K/Akt pathway. Eur J Pharmacol. 2023; 955: 175930. |
| 31 | Bi CF, Liu J, Hao SW, Xu ZX, Ma X, Kang XF, et al. Xuebijing injection protects against sepsis-induced myocardial injury by regulating apoptosis and autophagy via mediation of PI3K/Akt/mTOR signaling pathway in rats. Aging. 2023; 15(10):4374-90. |
| [1] | Huixin Zhao, Yiming Dong, Sijia Wang, Jiayuan Shen, Zhenju Song, Mingming Xue, Mian Shao. Comparison between sepsis-induced coagulopathy and sepsis-associated coagulopathy criteria in identifying sepsis-associated disseminated intravascular coagulation [J]. World Journal of Emergency Medicine, 2024, 15(3): 190-196. |
| [2] | Qing Zhao, Jinfu Ma, Jianguo Xiao, Zhe Feng, Hui Liu. Data driven analysis reveals prognostic genes and immunological targets in human sepsis-associated acute kidney injury [J]. World Journal of Emergency Medicine, 2024, 15(2): 91-97. |
| [3] | Jia Li, Jiazhen Luo, Tao Hu, Ling Cheng, Weiwei Shang, Li Yan. Impact of next-generation sequencing on antimicrobial treatment in immunocompromised adults with suspected infections [J]. World Journal of Emergency Medicine, 2024, 15(2): 105-110. |
| [4] | Weichao Ding, Wei Zhang, Juan Chen, Mengmeng Wang, Yi Ren, Jing Feng, Xiaoqin Han, Xiaohang Ji, Shinan Nie, Zhaorui Sun. Protective mechanism of quercetin in alleviating sepsis-related acute respiratory distress syndrome based on network pharmacology and in vitro experiments [J]. World Journal of Emergency Medicine, 2024, 15(2): 111-120. |
| [5] | Wei Zhou, Maiying Fan, Xiang Li, Fang Yu, En Zhou, Xiaotong Han. Molecular mechanism of Xuebijing in treating pyogenic liver abscess complicated with sepsis [J]. World Journal of Emergency Medicine, 2024, 15(1): 35-40. |
| [6] | Fei Zeng, Lingyun Cai, Luyao Guo, Meijuan Lan, Jiangshuyuan Liang, Peipei Gu. Pulmonary rehabilitation protocols in urgent lung transplantation patients [J]. World Journal of Emergency Medicine, 2024, 15(1): 47-51. |
| [7] | Miao Gan, Liang Zong, Xuezhong Yu, Jun Xu. The effect of prophylactic antibiotics in acute upper gastrointestinal bleeding patients in the emergency department [J]. World Journal of Emergency Medicine, 2023, 14(6): 442-447. |
| [8] | Jingyi Wang, Li Weng, Jun Xu, Bin Du. Blood gas analysis as a surrogate for microhemodynamic monitoring in sepsis [J]. World Journal of Emergency Medicine, 2023, 14(6): 421-427. |
| [9] | Yufang Lin, Fei’er Song, Weiyue Zeng, Yichi Han, Xiujuan Chen, Xuanhui Chen, Yu Ouyang, Xueke Zhou, Guoxiang Zou, Ruirui Wang, Huixian Li, Xin Li. Cardiopulmonary prognosis of prophylactic endotracheal intubation in patients with upper gastrointestinal bleeding undergoing endoscopy [J]. World Journal of Emergency Medicine, 2023, 14(5): 372-379. |
| [10] | Saifeng Chen, Xuewei Hao, Guo Chen, Guorong Liu, Xiaoyan Yuan, Peiling Shen, Dongfeng Guo. Effects of mesencephalic astrocyte-derived neurotrophic factor on sepsis-associated acute kidney injury [J]. World Journal of Emergency Medicine, 2023, 14(5): 386-392. |
| [11] | Mubing Qin, Yanxia Gao, Shigong Guo, Xin Lu, Qian Zhao, Zengzheng Ge, Huadong Zhu, Yi Li. Establishment and evaluation of animal models of sepsis-associated encephalopathy [J]. World Journal of Emergency Medicine, 2023, 14(5): 349-353. |
| [12] | Guoxin He, Ancong Xu, Xichong Yu, Fan Huang, Lei Su. Heat stroke alters hippocampal and cerebellar transmitter metabonomics [J]. World Journal of Emergency Medicine, 2023, 14(4): 287-293. |
| [13] | Jiafa Lu, Xin Wang, Linghao Chen, Xuedong Sun, Rui Li, Wanjing Zhong, Yajing Fu, Le Yang, Weixiang Liu, Wei Han. Unmanned aerial vehicle based intelligent triage system in mass-casualty incidents using 5G and artificial intelligence [J]. World Journal of Emergency Medicine, 2023, 14(4): 273-279. |
| [14] | Meng-meng An, Chen-xi Liu, Ping Gong. Effects of continuous renal replacement therapy on inflammation-related anemia, iron metabolism and prognosis in sepsis patients with acute kidney injury [J]. World Journal of Emergency Medicine, 2023, 14(3): 186-192. |
| [15] | Guang-qi Guo, Yan-nan Ma, Shuang Xu, Hong-rong Zhang, Peng Sun. Effect of post-rewarming fever after targeted temperature management in cardiac arrest patients: a systematic review and meta-analysis [J]. World Journal of Emergency Medicine, 2023, 14(3): 217-223. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||
