Bronchial rupture from penetrating, perforating, or compressive cervical or thoracic injuries can lead to complete tracheal, mainstem bronchial, or lobar bronchial detachment. Although rare in children, bronchial rupture presents significant risks, including dyspnea, respiratory failure, and potentially fatal airway obstruction, and is often overlooked or diagnosed late in clinical settings. Prompt diagnosis and intervention are prognostically crucial.[1,2] Between January 2013 and December 2023, four children (two male and two female) with bronchial rupture were admitted to the Pediatric Surgical Intensive Care Unit (ICU) at Children’s Hospital, Zhejiang University School of Medicine. Here, we share our experience of patient management.
The injury mechanisms of the four children included traffic accidents (two), falls from a height (one), and blunt impact injury (one). All injuries were classified as closed.
Patient 1 was an 8-year-old boy who presented to the emergency department (ED) 6 h after a traffic accident. Before admission, he had chest compressions, resulting in facial petechiae and subsequent rapid and labored breathing. Initial evaluation at a local hospital revealed bilateral pulmonary contusions and bilateral pneumothoraces (predominantly left-sided) with 80% lung compression on chest computed tomography (CT). On admission, his heart rate (HR) was 130 beats/min, respiratory rate (RR) was 55 breaths/min, and oxygen saturation (SpO2) was 95% with mask oxygen. Paradoxical respiration, diminished bilateral chest wall movements, and bilaterally reduced breath sounds were observed. An immediate left-sided thoracostomy with closed drainage was performed. Despite mask oxygen supplementation, the SpO2 decreased with worsening subcutaneous emphysema. Bronchial rupture was suspected, and thoracic surgery consultation was conducted after endotracheal intubation. Emergency thoracotomy revealed a 1-cm tear near the left mainstem bronchus-upper lobe bronchus junction, with almost complete separation. The lesion was suture-repaired. Ventilatory support was withdrawn 20 h postoperatively, with the patient breathing 34-46 breaths/min on mask oxygen. The patient was transferred from the ICU to a general ward on postoperative day (POD) 6. Follow-up chest radiography revealed no residual pneumothorax. He was discharged in good health on POD 13.
Patient 2 was a 4-year-10-month-old girl and admitted to the ED 11 h after crush injury by a heavy object. She complained of right upper limb and chest pain, and the exact injury site was unclear. A CT scan at a local hospital revealed a right-sided pneumothorax with 80% lung compression, an obscured right bronchial view, and multiple right-sided rib fractures. On admission, her HR was 132 beats/min, RR was 40 breaths/min, and SpO2 was 99% with mask oxygen. Subcutaneous emphysema was noted in the right chest wall, neck, and shoulder area, with left-sided tracheal deviation, pronounced tenderness over the right chest, and decreased breath sounds on the right compared with those on the left. Urgent chest radiography revealed tension pneumothorax on the right, with 80%-90% lung collapse, mediastinal emphysema, suspected right main bronchial rupture, and right-sided second and third rib fractures. Immediate right-sided chest tube insertion was followed by an emergency thoracotomy, revealing a 0.8-cm right upper lobe bronchial laceration below the carina, which was sutured intraoperatively. Ventilator withdrawal occurred 75 h postoperatively. Bronchoscopy on POD 10 revealed granulation tissue in the right main and intermediate bronchi. The patient was transferred from the ICU on POD 11 and discharged on POD 15.
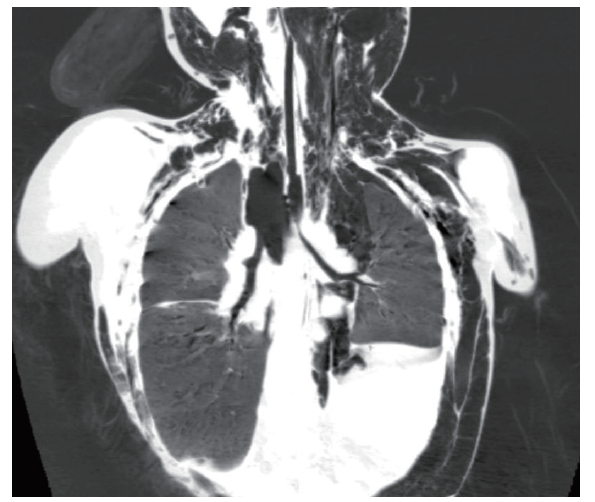
Patient 3 was a 4-year-old boy and admitted after being unconscious for more than a day following a car accident. A CT scan at a local hospital revealed a large right-sided pneumothorax, minor pleural effusion, extensive subcutaneous emphysema in the neck, chest, and abdominal wall, minimal mediastinal air, and exudative pulmonary changes. Chest tube insertion and mechanical ventilation were initiated. Owing to his critical condition, he was transferred to our hospital with an endotracheal tube in place. On arrival, he was unconscious, with coarse breath sounds and extensive rales bilaterally. Continuous right-sided chest drainage was performed. Management included ongoing mechanical ventilation, chest drainage, norepinephrine for blood pressure maintenance, and antibiotics. Worsening subcutaneous emphysema prompted a repeat chest radiograph, confirming increased extra-pulmonary gas accumulation. On day 5, CT suggested lower bronchial rupture (Figure 1). On day 6, exploratory surgery revealed complete right main bronchial transection at the carina. Under extracorporeal circulation, sleeve resection and tracheal and carinal reconstruction were performed via interrupted sutures with 3-0 absorbable threads. Ventilatory support was withdrawn on POD 5, and ICU discharge occurred on POD 12.
Figure 1.
Figure 1.
CT scan suggesting lower tracheal rupture of the patient 3. CT: computed tomography.
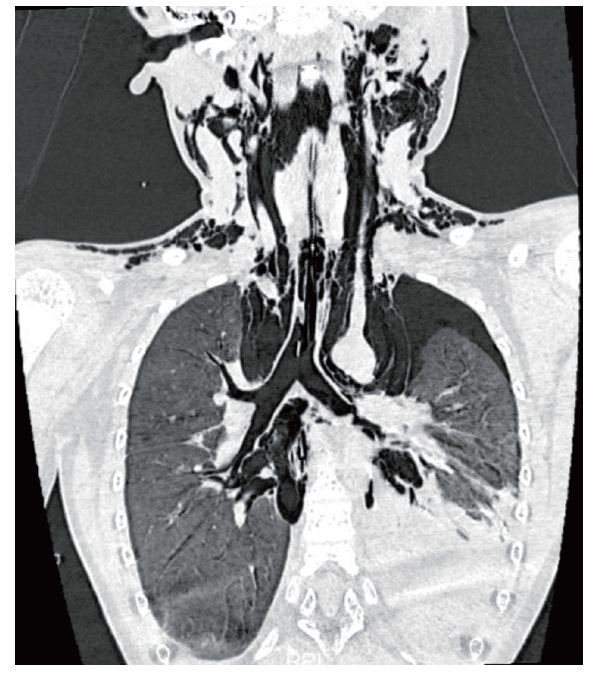
Patient 4 was an 8-year-6-month-old girl and admitted to the ED after a fall. Upon examination, her pulse was 132 beats/min, RR was 40 breaths/min, and SpO2 was 99% with ventilatory support. Cervical surgical emphysema was palpable, and breath sounds were reduced bilaterally. CT revealed a left lung contusion with extensive atelectasis, a large left-sided hemopneumothorax, a right lung contusion, mediastinal air, and subcutaneous emphysema in the anterior chest, neck, shoulders, back, and buttocks. Left-sided chest tube insertion, infection control, and other supportive treatments were initiated. A follow-up CT suggested possible distal left main bronchial rupture (Figure 2). On day 7, thoracotomy revealed a complete break in the left main bronchus, which was repaired via the sleeve technique. Ventilator support was withdrawn on POD 7, and bronchoscopy on POD 9 revealed inflammatory changes and postoperative bronchial reconstruction. The patient was transferred out of the ICU on POD 13.
Figure 2.
Figure 2.
Follow-up CT scan indicating potential rupture in the distal left main bronchus of the patient 4. CT: computed tomography.
All patients survived during their hospital stay. No patients developed postoperative bronchial anastomotic leaks, and successful weaning from mechanical ventilation was achieved in all patients. No further surgical interventions were necessary on the basis of postoperative follow-up assessments. Over follow-up periods ranging from 3 months to 10 years, the patient 2 experienced early bronchial stenosis episodes requiring frequent oxygen supplementation. The remaining patients had no significant respiratory infections or other functional respiratory abnormalities.
Thoracic trauma, particularly from motor vehicle accidents, is the primary cause of bronchial rupture. This trend, driven by economic development and increased vehicle use, suggests a potential rise in pediatric cases, which aligns with the previous literature.[3]
The mechanisms of bronchial rupture can be categorized as follows: bilateral bronchi experiencing lateral traction leading to rupture at the carina when the thorax undergoes significant external force, increased airway pressure due to vocal cord closure and breath-holding during chest and airway impact, and direct force applied to fixed points over the bronchi.[4] Herein, bronchial ruptures in our patients occurred within 2.5 cm of the carina, which is consistent with Cheaito’s report suggesting that the right main bronchus is more susceptible to rupture,[5] although our findings mirror those of Kiser’s,[6] indicating equal likelihood for both sides.
Patients with severe chest trauma whose tension pneumothoraces and lung collapse persist despite closed chest drainage and mechanical ventilation, respectively, pose challenges. Radiographically, a characteristic “fallen lung” sign may be indicative;[7] however, prompt CT with airway reconstruction is advisable when feasible, as CT imaging and virtual bronchoscopy increase the diagnostic accuracy to 94%-100%.[8] Patients 3 and 4 revealed bronchial rupture on CT with airway reconstruction. Fiberoptic bronchoscopy is the gold standard for diagnosis and surgical guidance. Its wide availability has proven valuable,[9]with bronchoscopic findings matching intraoperative observations regarding rupture location and length. Although only one preoperative bronchoscopy was performed in our patients without conclusive rupture identification, intraoperative bronchoscopic guidance was used for intubation in all patients. Preoperative bedside bronchoscopy is now considered feasible and appropriate. Moreover, postoperative bronchoscopy aids in monitoring inflammation, infection, and granulation tissue formation.[3]
Prompt thoracostomy with closed drainage is crucial for managing massive pneumothoraces, especially in closed injuries, as it immediately alleviates tension pneumothoraces and helps assess trauma severity. All four patients in this study required mechanical ventilation to maintain vital signs. Immediate surgical intervention is imperative for pediatric bronchial ruptures,[10] as conservative management exacerbates this condition. After conservative therapy, patients 3 and 4 were found to have complete bronchial transections intraoperatively, with the patient 3 requiring extracorporeal membrane oxygenation support for repair. Postoperative management included mechanical ventilation, enhanced respiratory care, antimicrobial therapy, and maintenance of chest drain patency.
In conclusion, although rare, bronchial rupture in children poses significant risks, emphasizing the need for prompt diagnosis and intervention. Selective CT with 3D reconstruction is advisable when patients are hemodynamically stable. Bedside fiberoptic bronchoscopy, when available, is an invaluable diagnostic tool. An aggressive surgical strategy is imperative for strong suspicion or confirmation. Integrating fiberoptic bronchoscopy preoperatively, intraoperatively, and postoperatively significantly enhances the assessment and management of bronchial disruptions, thereby optimizing patient outcomes.
Funding: None.
Ethical approval: The study adhered to the principles of the Declaration of Helsinki and was approved by the Ethics Committee of Children’s Hospital, Zhejiang University School of Medicine (approval number: 2024-IRB-0128-P-01).
Conflicts of interest: The authors declare that they have no conflicts of interest.
Contributors: YYB: data collection, visualization, manuscript writing (original version, manuscript writing - edits and revision); JY, LJG, CNG, and LH: literature search, data collection; LHT: manuscript writing (original version, manuscript writing, edits, and revision). All authors contributed significantly to the manuscript, read and approved the final version of the manuscript.
Reference
Experience of diagnosis and treatment of traumatic bronchial rupture in children in a single clinical center
DOI:10.1007/s00383-020-04703-2
PMID:32572599
[Cited within: 1]

To examine the diagnosis and treatment of traumatic bronchial rupture in children at the Children's Hospital of Chongqing Medical University, Chongqing, China.The diagnosis and treatment of eight cases of traumatic bronchial rupture were analyzed retrospectively from January 2014 to December 2019 in our hospital.Diagnosis of the eight patients was clear after a chest CT with three-dimensional reconstruction techniques and fiberoptic bronchoscopy; six of the patients had a delay in diagnosis of at least 2 weeks. Among the patients, six had left bronchus rupture, and the other two had right bronchus rupture. All eight patients received surgery; seven patients received a bronchial end-to-end valgus anastomosis, and one received right middle lobe lobectomy. There were no deaths in this group, and all patients were cured and discharged. Follow-up was conducted for 3 months to 2 years; the patients who received surgery showed mild bronchostenosis within 2 weeks after the trauma, and the other six patients showed moderate bronchostenosis upon CT examination.Being alert to bronchial rupture after trauma in children is helpful for diagnosis. Chest CT with three-dimensional reconstruction techniques and fiberoptic bronchoscopy are the most valuable diagnostic methods. The patients can show excellent results if the operation for a continuous valgus anastomosis of the posterior wall and interrupted end-to-end valgus anastomosis of the anterior wall on the ruptured side is performed in the early stage of traumatic bronchial rupture.
Hepatic rupture secondary to HELLP syndrome: outcomes in three cases
DOI:10.5847/wjem.j.1920-8642.2024.003 PMID:38188560 [Cited within: 1]
Blunt traumatic bronchial rupture in patients younger than 18 years
Management of tracheobronchial disruption secondary to nonpenetrating trauma
PMID:779688
[Cited within: 1]

The pathogenesis, pathology, clinical presentation, diagnosis and management of tracheo-bronchial injuries secondary to nonpenetrating thoracic trauma are discussed.
Traumatic bronchial injury
Blunt tracheobronchial injuries: treatment and outcomes
DOI:10.1016/s0003-4975(00)02453-x
PMID:11426809
[Cited within: 1]

Tracheobronchial injury is a recognized, yet uncommon, result of blunt trauma to the thorax. Often the diagnosis and treatment are delayed, resulting in attempted surgical repair months or even years after the injury. This report is an extensive review of the literature on tracheobronchial ruptures that examines outcomes and their association with the time from injury to diagnosis.We reviewed all patients with blunt tracheobronchial injuries published in the literature to determine the anatomic location of the injury, mechanism of the injury, time until diagnosis and treatment, and outcome. Only patients with blunt intrathoracic tracheobronchial traumas were included.We identified 265 patients reported between 1873 and 1996. Motor vehicle accidents were the most frequent mechanism of injury (59%). The overall mortality among reported patients has declined from 36% before 1950 to 9% since 1970. The injury occurred within 2 cm of the carina in 76% of patients, and 43% occurred within the first 2 cm of the right main bronchus. The proximity of the injury to the carina had no detectable effect on mortality. Injuries on the right side were treated sooner but were associated with a higher mortality than left-sided injuries. No association was detected between delay in treatment and successful repair of the injury; ninety percent of patients undergoing treatment more than 1 year after injury were repaired successfully.This review of patients with blunt tracheobronchial injuries represents the largest cohort studied to date. These data suggest an ability to repair tracheobronchial injuries successfully many months after they occur. We are also able to assess the mortality associated with the location and side of injury, examine the time from injury until diagnosis and treatment, and evaluate treatment outcome.
Management of tracheobronchial injuries
DOI:10.21037/jtd-2019-as-05
PMID:33209452
[Cited within: 1]

Tracheobronchial injuries (TBI) are a heterogenous group of sometimes life-threatening traumas with different management approaches. Symptoms are mediastinal and subcutaneous emphysema, bloody secretions from the airway or haemoptysis in alert patients, and high air leakage along the cuff or increased ventilatory resistance may be signs for TBI in intubated patients. The necessity of immediate clinical evaluation, CT-scan and bronchoscopic evaluation are essential for prompt diagnosis and classification as well as experienced air way management and treatment, these patients are best managed from interdisciplinary teams including thoracic surgeons. While iatrogenic tracheal membrane laceration from intubation can be treated by lesion bridging with ventilation tube, stent application, open operative repair or endoluminal repair, intraoperative accidental cuts should be repaired by direct suture or with vital tissue coverage in case of local ischemia. The management of blunt or penetrating injury is sequential and needs immediate establishment and maintenance of a secure patent airway to provide adequate oxygenation. The next step is the treatment of life-threatening collateral injuries like major hemorrhage, cranial trauma or major organ damage arranged in the trauma team. The treatment of penetrating injuries to the airway need operative exploration in almost every case with minimal local dissection and debridement followed by direct repair. Muscle flap coverage is useful in case of combined esophageal injury. Damage of the tracheobronchial tree after blunt trauma must be repaired by direct suture or local tissue sparing resection and anastomosis. These lesions can be missed in the initial phase and may become prominent with scar tissue formation, stenosis and atelectasis in the later phases.2020 Journal of Thoracic Disease. All rights reserved.
Airway trauma: a review on epidemiology, mechanisms of injury, diagnosis and treatment
DOI:10.1186/1749-8090-9-117
PMID:24980209
[Cited within: 1]

Airway injuries are life threatening conditions. A very little number of patients suffering air injuries are transferred live at the hospital. The diagnosis requires a high index of suspicion based on the presence of non-specific for these injuries symptoms and signs and a thorough knowledge of the mechanisms of injury. Bronchoscopy and chest computed tomography with MPR and 3D reconstruction of the airway represent the procedures of choice for the definitive diagnosis. Endotracheal intubation under bronchoscopic guidance is the key point to gain airway control and appropriate ventilation. Primary repair with direct suture or resection and an end to end anastomosis is the treatment of choice for patients suffering from tracheobronchial injuries (TBI). The surgical approach to the injured airway depends on its location. Selected patients, mainly with iatrogenic injuries, can be treated conservatively as long as the injury is small (<2 cm), a secure and patent airway and adequate ventilation are achieved, and there are no signs of sepsis. Patients with delayed presentation airway injuries should be referred for surgical treatment. Intraoperative evaluation of the viability of the lung parenchyma beyond the site of stenosis/obstruction is mandatory to avoid unnecessary lung resection.
Reverse turnover pedicled latissimus dorsi muscle flap for lower back reconstruction: two case reports
Posttraumatic main left bronchial rupture