Trousseau syndrome is characterized by thromboembolism induced by malignancy[1] and typically affects middle-aged to elderly patients.[2⇓-4] When faced with a young patient suffering from cerebral infarction and diffuse arterial emboli, there is some controversy regarding whether to consider it a concurrent malignancy triggering Trousseau syndrome or to adhere to TOAST (Trial of Org 10172 in Acute Stroke Treatment) for common causes.[5,6] In this case study, we aimed to report a young patient with Trousseau syndrome presenting with multiple arterial emboli.
A 27-year-old male patient with a history of smoking for more than a decade (20 cigarettes per day) had been experiencing intermittent chest discomfort for the past half year without any other notable medical history, such as HIV. While undergoing treatment at a local emergency department for acute abdominal pain and diarrhea, the patient suddenly lost consciousness during the administration of intravenous normal saline. An emergent head computed tomography (CT) scan revealed no abnormalities; however, a follow-up head scan on the next day revealed multiple and massive cerebral infarcts. Consequently, the patient was transferred to the Intensive Care Unit of Guangdong Provincial People’s Hospital for further diagnosis and treatment.
His vital signs were normal, with an oxygen saturation level of 99%. The skin of the nasal tip, earlobes, left index finger and left lower limb exhibited cyanosis, while no facial, neck, or limb swellings were present. Auscultation of the chest revealed suppressed breath sounds and lung crackles, while auscultation of the heart indicated a diminished heart tone. Neurological examination revealed a Glasgow Coma Scale score of E1VTM4, decreased muscle strength (the left limb [grade 2/5] and the right limb [grade 0/5]) and a positive Babinski reflex on both sides. All other neurological, chest and abdominal examinations were normal.
The results of immediate arterial blood gas analysis were normal. Laboratory examination revealed thrombocytopenia (platelet level 43×109/L), elevated total leukocyte counts (20.96×109/L) and neutrophil counts (16.69×109/L), procalcitonin 43×109/L, C-reactive protein (CRP) 68.9 mg/L, interleukin-6 (IL-6) 41.4 pg/mL, impaired liver and renal function (aspartate transaminase [AST] 666 U/L, alanine aminotransferase [ALT] 500 U/L, and serum creatinine [Scr] 93.43 μmol/L), abnormal coagulation (international normalized ratio [INR] 1.37, prothrombin time [PT] 16.9 s, fibrinogen [FIB] 1.55 g/L, activated partial thromboplastin time [APTT] 43.3 s, D-dimer >20,000 ng/mL, antithrombin III activity 78%, protein C activity 31%, protein S activity 41% and lupus anticoagulant ratio 1.07) and elevated tumor markers (neuron-specific enolase 22.99 ng/mL, carcinoembryonic antigen 268.47 ng/mL). The results of routine urine tests were normal. An examination of autoimmune assays revealed no abnormalities. Screening for infectious diseases, including HIV, syphilis, hepatitis and tuberculosis, yielded negative results. Admission CT scans with contrast enhancement revealed, in addition to multiple large areas of cerebral infarction, the presence of pulmonary embolism, renal infarction, splenic infarction and multiple arterial occlusions in the left lower limb. However, neither CT nor ultrasound scans revealed the presence of deep vein thrombosis. Furthermore, there was bilateral pleural effusion and a substantial amount of pericardial effusion (Figure 1). The echocardiogram also revealed significant pericardial effusion and mild aortic regurgitation.
Figure 1.
Figure 1.
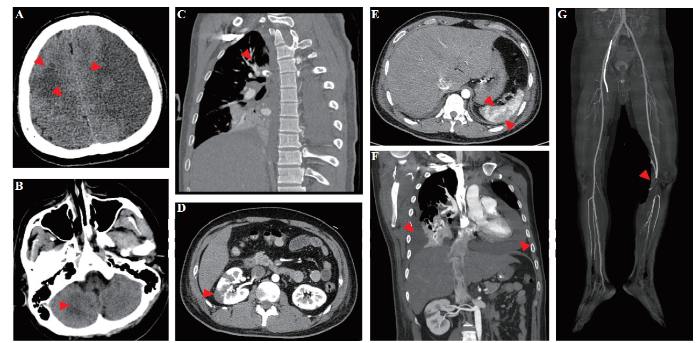
Multiple organ infarctions on computed tomography (CT). A-B: multiple and massive cerebral infarction (red arrows); C: pulmonary embolism (red arrow); D: renal infarction (red arrow); E: splenic infarction (red arrow); F: pleural effusion and pericardial effusion (red arrows); G: interruption of arterial blood flow of left lower extremity (red arrow).
Given the patient’s critical condition, hypercoagulable state, and pleural and pericardial effusions, a multidisciplinary consultation was promptly organized. Further examinations were conducted as advised, including tests for antibodies against beta 2-glycoprotein 1 (IgA, IgG, IgM), anti-cardiolipin antibodies (IgA, IgG, IgM), and lupus anticoagulant, all of which returned negative results. Additionally, a positron emission tomography/computed tomography (PET/CT) scan revealed a 15 mm×12 mm high-metabolic lesion in the apical segment of the right upper lung. Cytopathological examination of the pleural and pericardial effusions revealed the presence of adenocarcinoma cells, with immunophenotypic analysis attributing their origin to the lung. Following consultation with the pulmonary oncology department, a diagnosis of adenocarcinoma in the apical segment of the right upper lung was confirmed. On this basis, a clear diagnosis of Trousseau syndrome, which is characterized by three-territory sign (TTS), widespread arterial thromboembolism, lung adenocarcinoma and significantly elevated D-dimer levels, was established. Following anticoagulation therapy, targeted treatments and comprehensive management, the patient regained consciousness. However, his left lower limb extremity developed necrosis, and finally could not avoid amputation. At the half-year follow-up after discharge, the patient was alive with no new incidents of vascular thrombosis.
Trousseau syndrome was first described by Armand Trousseau in 1865 as thrombotic phlebitis in the context of cancer, and it was later expanded in 1977 to encompass venous or arterial thromboembolic events associated with malignant tumors.[1] Its clinical features include significantly elevated D-dimer levels, multi-focal cerebral infarctions (most prevalent and representative), as well as widespread venous and/or arterial thromboses throughout the body, usually affecting the pulmonary and peripheral arteries.[3]
Clinical examination revealed that when a patient presents with multi-regional cerebral infarctions, it is imperative to ascertain whether there is an underlying malignant tumor.[1,7,8] Indeed, vascular thrombosis may even be the primary clinical manifestation in patients with cancer.[1,9] The pathogenic mechanism may be associated with hypercoagulability induced by mucin production, which is typical of adenocarcinomas.[4] Consequently, management primarily involves anticoagulation therapy, with recommendations favoring the use of unfractionated heparin or low-molecular-weight heparin.[1,4]
In the present case, a young male patient with no significant medical history presented with loss of consciousness following two days of abdominal pain and diarrhea. Comprehensive screening revealed not only multi-focal cerebral infarcts with markedly elevated D-dimer levels but also pleural and pericardial effusions alongside abnormal levels of tumor markers, prompting thorough tumor localization and characterization and ultimately revealing concealed lung adenocarcinoma. Ultimately, the patient was diagnosed with Trousseau syndrome secondary to lung adenocarcinoma and successfully treated with anticoagulation and targeted therapies. This case also revealed the uncommon occurrence of renal and splenic infarcts associated with the syndrome. Tracing back, while abdominal pain was the initial symptom accompanied by diarrhea, a possible connection to renal and splenic infarction could not be definitively ruled out.
Moreover, the present case involved a young male, whereas the overwhelming majority of reported Trousseau syndrome cases concerned middle-aged to elderly individuals.[2⇓-4] In actual clinical practice, patients within this age range are infrequently suspected of having malignant tumors, as the probability of developing cancer is significantly lower in this demographic population compared with older adults.[10] In hindsight, the patient reported intermittent chest tightness in the precordial region for the past six months, indicating that pericardial effusion might have been present but was overlooked due to inadequate patient awareness. Timely medical examination could have potentially prevented this severe cerebrovascular incident. Similarly, given the patient’s young age, we did not initially consider malignancy as a top differential diagnosis. Furthermore, for certain reasons, the lung tumor was not detected on the contrast-enhanced CT of the chest, which was completed on the day of admission. The age of onset for lung cancer is decreasing, and early comprehensive cancer screening is advised for patients who present with arterial or venous thrombosis.[11] Fortunately, the present authors initiated multidisciplinary consultations early on, conducted a thorough investigation, quickly completed tumor screenings of the effusions, and carried out whole-body PET-CT, ultimately leading to a definitive diagnosis.
In conclusion, Trousseau syndrome is a rare condition that poses a diagnostic and therapeutic challenge to clinicians. When young patients present with TTS of unclear etiology, clinicians should maintain a high level of suspicion for concurrent malignancy and Trousseau syndrome, which can be induced by the malignancy.
Funding: None.
Ethical approval: The study was approved by the Ethics Committee of Guangdong Provincial People's Hospital (GDREC2018424H [R1]).
Conflicts of interest: We declared no competing interests.
Contributors: All authors were responsible for data curation and analysis. LQH and HKZ were responsible for supervision and validation. LQH and YW wrote the original draft. All authors contributed to review and editing of the report.
Reference
Multiple cerebral infarction linked to underlying cancer: a review of Trousseau syndrome-related cerebral infarction
Trousseau syndrome related cerebral infarction: clinical manifestations, laboratory findings and radiological features
Cerebral infarction caused by Trousseau syndrome associated with cervical cancer
Prognosis of pancreatic cancer with Trousseau syndrome: a systematic review of case reports in Japanese literature
Predicting acute myocardial infarction during acute ischemic stroke: need for a screening tool beyond biomarkers
Prediction of acute myocardial infarction in asian patients with acute ischemic stroke: the CTRAN score
Stroke as initial manifestation of non-small cell lung cancer with Trousseau syndrome
A case of Trousseau syndrome: screening, detection and complication
Cancer-related coagulopathy (Trousseau’s syndrome): review of the literature and experience of a single center of internal medicine
Cancer incidence and mortality in China, 2022
Systematic review: the Trousseau syndrome revisited: should we screen extensively for cancer in patients with venous thromboembolism?